Chronic Venous Insufficiency occurs when your leg veins are unable to push blood back up to the heart as they should. Valves get damaged, blood backs up, pools in the lower legs, and pressure builds. This leads to swelling, aches, skin changes, and, in some cases, ulcers.
Struggling with swelling, fatigue, or post-surgery recovery?
Book your personalized lymphatic drainage session today and experience natural, therapeutic healing that restores balance and promotes long-term wellness.
Book an AppointmentIt often follows a deep vein thrombosis, years of standing on the job, or simply the natural aging process. Many people live with CVI without realizing how much better they could feel. If your legs feel heavy by the end of the day or you notice bulging veins, this guide can help stop things from getting worse.
What is Chronic Venous Insufficiency?
Chronic Venous Insufficiency starts with faulty one-way valves in the leg veins. Typically, the valves prevent blood from moving downward against gravity. When they weaken, blood flows backward, pools, and creates high pressure in the veins.
That pressure forces fluid out into the tissues, causing swelling and inflammation. Over time, veins stretch and become varicose, while the surrounding skin and fat are damaged due to a lack of oxygen and nutrients. CVI also overloads the nearby lymphatic system, making it more challenging to clear swelling and setting the stage for more severe problems.
How CVI Affects the Lower Legs
In the lower legs and ankles, Chronic Venous Insufficiency causes a familiar, heavy, and tired feeling, especially after prolonged periods of standing or sitting. Ankles swell up, the skin turns darker or thicker from leaked blood pigments, and simple activities like walking longer distances start to hurt. If the pressure stays high, open sores become a real risk.
Chronic Venous Insufficiency Causes
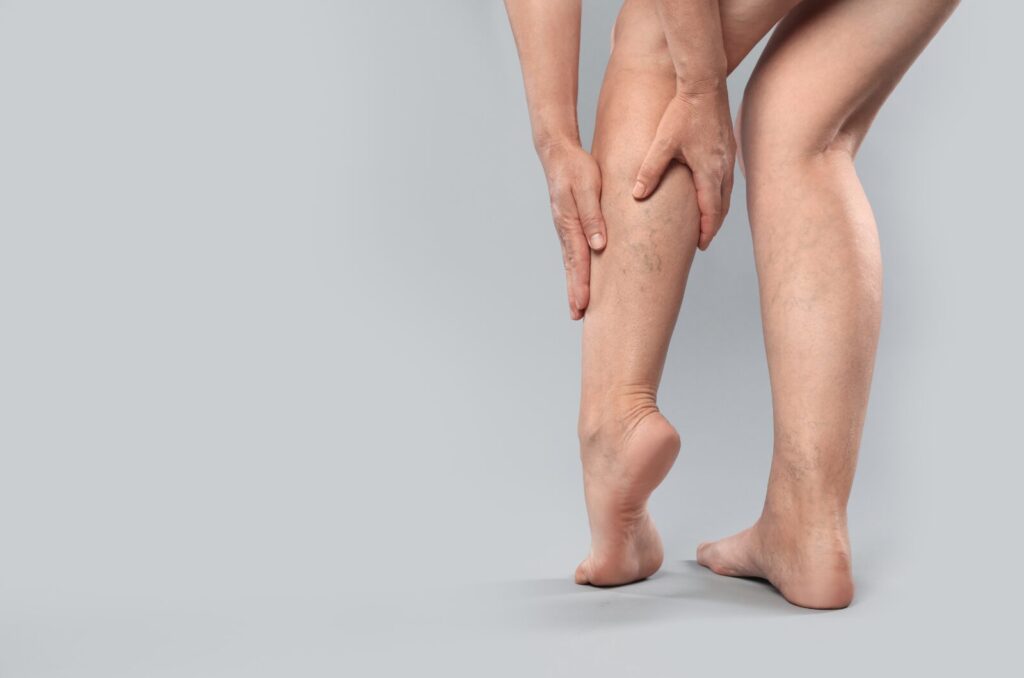
The main Chronic Venous Insufficiency can be narrowed down to anything that damages the vein valves, either from birth defects or from damage later in life, often from a blood clot that scars the vein.
Daily habits pile on: jobs that keep you on your feet for hours, extra weight pressing down, or sitting too long without moving. Smoking weakens vessel walls, and repeated inflammation slowly breaks things down further.
Common Risk Factors
The biggest risks for Chronic Venous Insufficiency include being over 50, multiple pregnancies, family history of vein problems, and lack of regular movement. Tall people, smokers, and anyone carrying extra pounds face higher odds, too.
Early and Advanced Chronic Venous Disease Symptoms
Chronic Venous Disease Symptoms creep up gradually, starting mild and getting serious if ignored. Knowing the stages helps catch it early.
Step 1 — Early Symptoms to Watch For
The first clues are swollen ankles that puff up by evening, legs feeling heavy or achy after activity, and quick fatigue. Spider veins appear, with some faint, brownish tint near the ankles.
Step 2 — Progressing Symptoms
Next comes thicker skin, reddish-brown staining from blood leaking out, and that tight, itchy feeling. High pressure can cause fluid to seep through the skin, resulting in wet patches or crusty areas.
Step 3 — Advanced and Complicated Symptoms
At its worst, constant inflammation hardens tissues, ulcers form and refuse to heal, and infections can easily set in. The lymphatic system becomes overwhelmed, leading to lymphedema or combined phlebo-lymphedema, which causes the legs to balloon even more. Catching these Chronic Venous Insufficiency warning signs early keeps most people from ever reaching this point.
How CVI and Lymphedema are Linked
Chronic Venous Insufficiency puts constant back-pressure on the veins, which spills over to the lymphatic vessels trying to clean up excess fluid. When the lymph system can’t keep up, you get secondary lymphedema on top of the venous swelling. This is called phlebo-lymphedema.
Without addressing the venous flow, swelling persists, the skin thickens more rapidly, and healing wounds become almost impossible to manage. Getting circulation moving again takes the load off the lymphatics and stops the downward spiral.
Diagnosing Chronic Venous Insufficiency
Diagnosing Chronic Venous Insufficiency begins with a simple office examination, which involves assessing your legs both standing and lying down, checking for swelling, color changes, or noticeable varicose veins. Other effective diagnosis methods include:
Clinical Evaluation
Your doctor will ask about symptoms, family history, and daily habits while inspecting skin texture and feeling for tender spots.
Medical Tests
The gold standard for diagnosis is duplex ultrasound, which uses painless sound waves to visualize blood flow in the wrong direction or blocked areas. Sometimes deeper imaging rules out other issues.
Importance of Early Diagnosis
Spotting CVI sooner makes treatment simpler and prevents irreversible damage, such as ulcers or permanent corneal thickening.
Chronic Venous Insufficiency Treatment Options
Chronic Venous Insufficiency Treatment centers on moving fluid out, protecting skin, and supporting better flow. A mix of approaches works best for most people.
Complex Decongestive Therapy (CDT)
Complete CDT therapy packages include manual drainage, bandaging, exercises, and skin care. This helps drop swelling fast.
Manual Lymph Drainage
Manual lymphatic drainage employs gentle, rhythmic strokes to gently guide trapped fluid toward the lymph nodes that are actively working.
Compression Bandaging and Garments
Short-stretch bandages or medical compression stockings provide steady pressure, which helps veins push blood upward.
Exercise and Movement Therapy
Simple calf pumps, walking programs, or ankle circles build natural vein support.
Nutrition and Diet Management
Cutting back on salt, eating anti-inflammatory foods, and maintaining a healthy weight all help ease the burden on veins.
Self-Care Strategies
Daily leg elevation, moisturizing, and avoiding prolonged periods of stillness help reduce flare-ups. These steps directly tackle Chronic Venous Insufficiency and give day-to-day relief.
Goals of Treatment and Long-Term Management
Chronic Venous Insufficiency Treatment is designed to help you return to your normal daily activities without experiencing constant leg trouble.
Reducing Swelling and Edema
Consistent compression therapy and drainage shrink the puffiness that makes shoes tight and legs tired.
Improving Skin Health and Preventing Wounds
Better circulation, combined with good skincare, helps prevent discoloration, dryness, and those hard-to-heal ulcers.
Increasing Mobility and Comfort
Stronger vein support means you can walk farther without aching or feeling heavy.
Reducing Pain, Tightness, and Discomfort
Targeted therapies quiet the throbbing, burning, or restless feelings that disrupt sleep and daily life. Sticking with habits long-term keeps these wins in place.
Conclusion
Chronic Venous Insufficiency can disrupt your comfort, starting with tired legs and potentially ending in stubborn swelling, skin damage, or ulcers that won’t heal. Knowing CVI causes, such as valve failure, standing jobs, or past clots, helps you spot risks early. Symptoms progress in clear stages, but proven treatments, such as compression, manual drainage, exercise, and lifestyle adjustments, can turn things around and prevent irreversible complications.
At Lymphatic Therapy Services, we specialize in combining these approaches to reduce swelling, promote skin healing, and restore easy movement. Don’t let leg heaviness become your norm. Contact us today for an evaluation and start feeling lighter on your feet again.
FAQs
What Are The First Signs of Chronic Venous Insufficiency?
The earliest signs of Chronic Venous Insufficiency include swollen ankles at the end of the day, a heavy or achy feeling in the legs after standing, and possibly visible spider veins. Nighttime cramps or restless legs can also occur, often easing when you elevate your feet.
What Causes Chronic Venous Insufficiency to Develop?
It mainly comes from damaged valve structures that let blood flow backward and pool. Common triggers include previous deep vein clots, long hours standing or sitting, extra weight, pregnancies, smoking, or family genetics, making veins weaker over time.

