Living with fat disorders, such as lipedema, Dercum’s disease, MADL, or other rare adipose conditions, means waking up every day to painful, heavy, and bruised limbs that no diet or workout can shrink. The legs, arms, hips, and sometimes trunk swell with abnormal fat that feels hard and tender.
Struggling with swelling, fatigue, or post-surgery recovery?
Book your personalized lymphatic drainage session today and experience natural, therapeutic healing that restores balance and promotes long-term wellness.
Book an AppointmentDoctors dismiss it, strangers judge, clothes don’t fit, and shame becomes constant. Strong emotional support is not a luxury; it’s a necessity for survival. It lowers inflammation, cuts pain flares, ends isolation, rebuilds hope, and reminds every person they are still worthy of love exactly as they are.
Understanding Fat Disorders and Their Emotional Impact
What fat disorders are
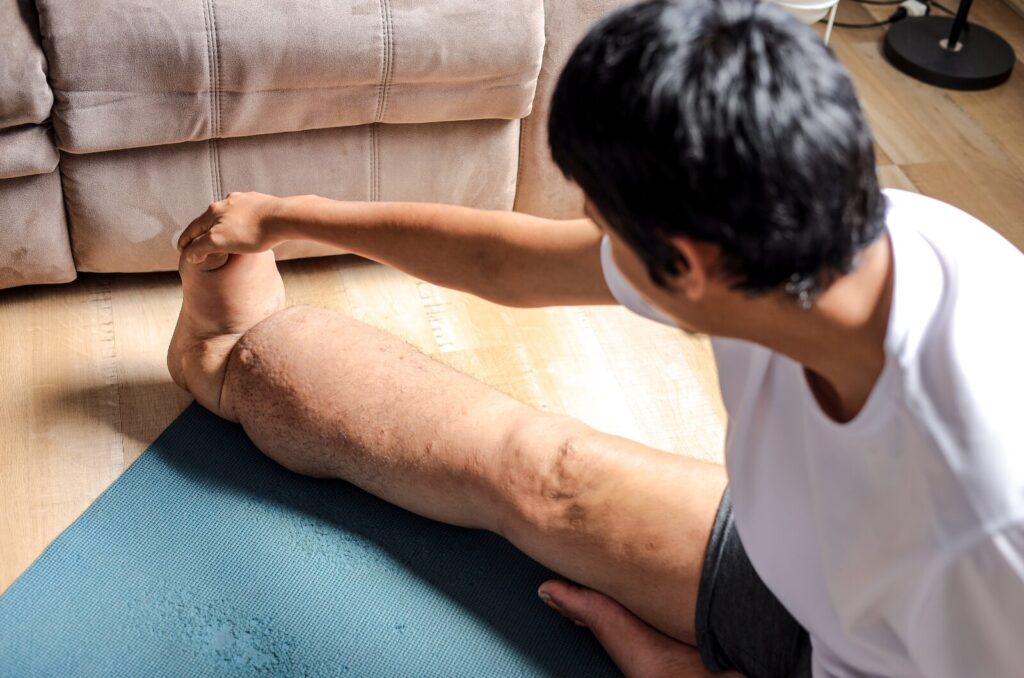
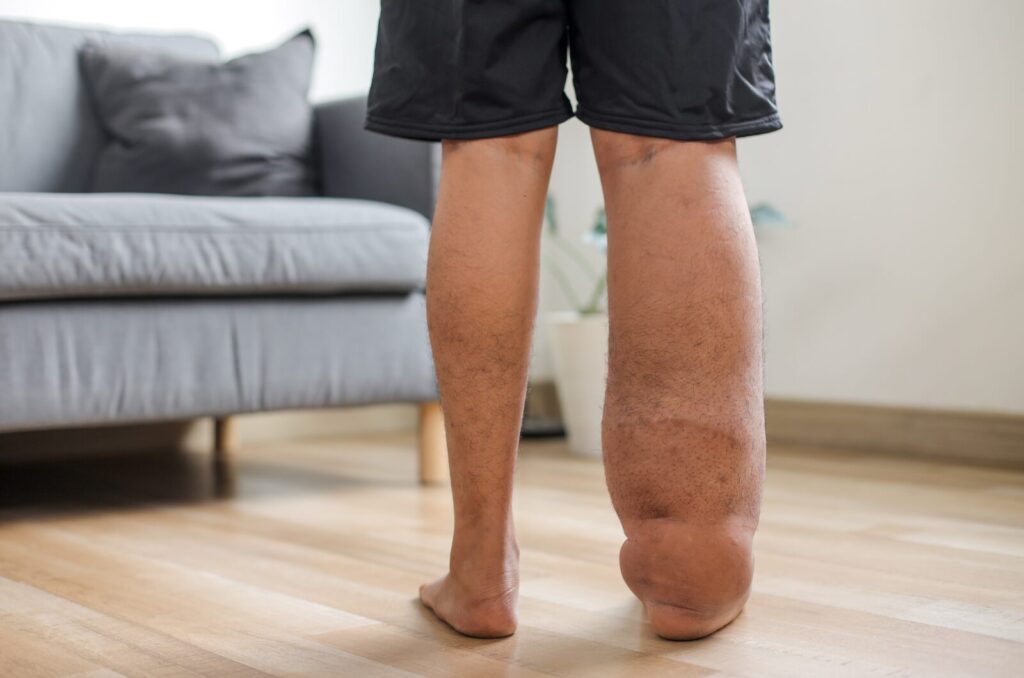
Fat disorders are medical conditions characterized by abnormal, often painful fat deposits that accumulate in specific areas of the body. The most commonly affected areas are the legs, hips, arms, and trunk. Lipedema is the best-known, affecting many people (primarily women), but Dercum’s disease (hundreds of painful lumps), MADL, and familial multiple lipomatosis also exist. These are genetic or hormonal, not lifestyle-driven, and regular weight-loss methods fail.
How symptoms affect daily life and self-image
Heavy, easy-to-bruise limbs make every step, stair, or long sit hurt. Simple tasks, such as grocery shopping, playing with kids, or getting dressed, become exhausting battles. Mirrors turn into enemies, favorite clothes get cut up for comfort, and the body feels like a stranger that betrayed you despite every effort.
Emotional challenges: frustration, isolation, body shame
Years of hearing “just eat less and move more” when nothing works creates rage and despair. Friends drift away, partners don’t understand, and many hide under baggy clothes or skip weddings, beaches, and photos. The shame feels heavier and more painful than the limbs themselves.
Why People with Fat Disorders Need Emotional Support

Chronic pain and mobility issues affect mental health
Constant burning, aching, and heaviness steal joy and energy. When walking to the mailbox hurts, or you can’t keep up with your own kids, feelings of worthlessness creep in fast. Emotional support fights hopelessness, reminds people that their value isn’t measured by pain levels, and provides a space to grieve without judgment.
Social stigma and misunderstanding surrounding fat disorders
Doctors, coworkers, and family regularly call fat disorders lipedema plain obesity. Being blamed for a medical condition you didn’t choose feels like a punch every time. The repeated dismissal pushes people into silence and loneliness; no one believes the pain is real.
The psychological cycle of stress, pain, and symptom flare-ups
Stress tightens muscles, raises cortisol, and spikes inflammation, making the fat tissue hurt and swell even more. More pain creates more stress, trapping people in a brutal loop. Steady, understanding support lowers stress hormones, calms the body, and dramatically reduces the frequency and intensity of flare-ups.
How Emotional Support Improves Coping and Quality of Life
Building resilience and reducing emotional distress
When someone finally says, “I see you, I believe you, this isn’t your fault,” the emotional weight lifts instantly. Feeling truly understood lowers anxiety, depression, and the dark thoughts that haunt too many in the fat disorders lipedema community. Hope returns, and fighting feels possible again.
Increased motivation toward treatment and self-care
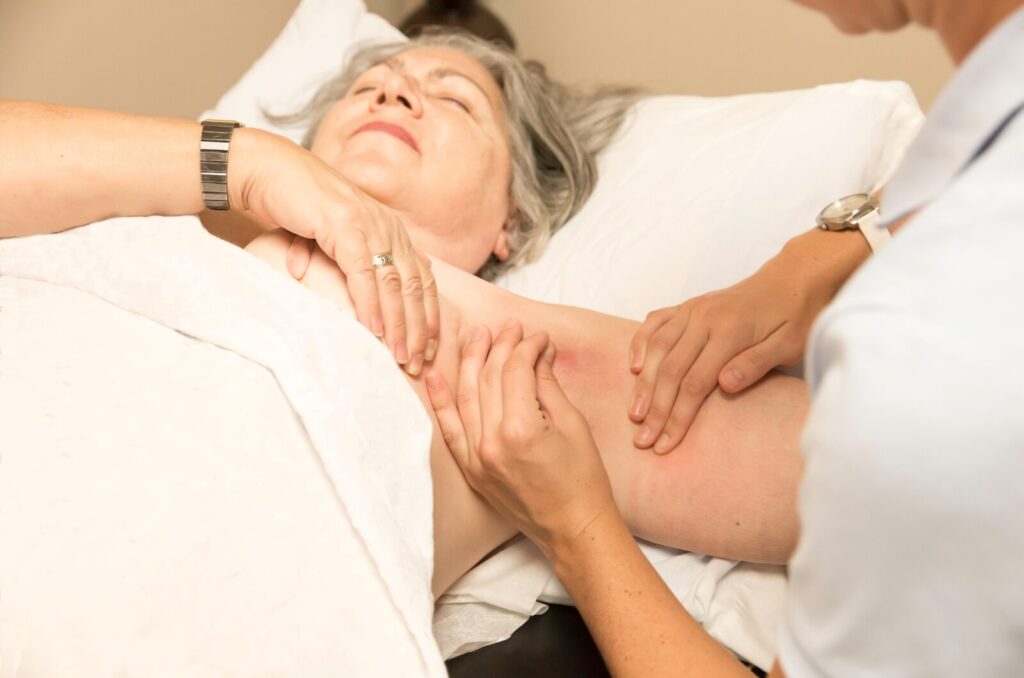
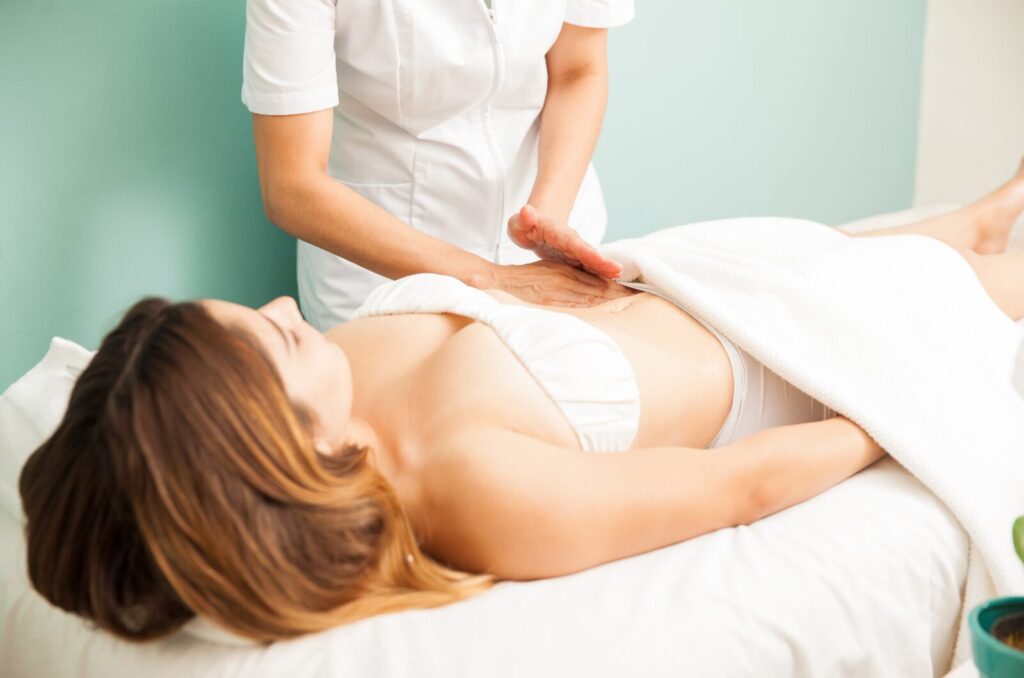
Support from others who have experienced it keeps patients motivated to undergo lymphatic massage, wear compression daily, try new therapies, and fight insurance denials, even when progress is slow and setbacks are tough. Knowing you’re not alone makes the effort feel worth it.
Improved body acceptance and reduced guilt or shame
Hearing dozens of stories about identical legs, identical bruises, and identical struggles shifts the blame from “I’m a failure” to “I have a tough condition.” Many finally look in the mirror without hating what they see and start treating their body with kindness instead of punishment.
Emotional Support Techniques That Help People Cope
Mindfulness and stress reduction practices
Five-minute deep breathing exercises, body scans, or guided meditations can help reduce cortisol levels quickly and effectively. Many women notice a reduction in burning and heaviness in their legs the same day they practice. This is clear proof that a calmer mind directly helps the painful bodies living with fat disorders.
Journaling and emotional expression
Writing about anger, grief, small victories, or doctor frustrations helps release the poison instead of letting it build up. Reading old entries later shows real progress, reminds people of their strength, and keeps hope alive on the darkest days.
Cognitive reframing to challenge negative thoughts
Switching “my legs are disgusting” to “my legs are fighting a medical condition and still carry me every day” feels fake at first. After weeks of practice, the inner critic quiets, self-compassion grows, and shame loses its grip.
Conclusion
Emotional support isn’t just helpful for people with fat disorders Lipedema. It’s often the difference between giving up and keeping going. It reduces daily pain, breaks the vicious cycle of stress and pain, rebuilds self-worth, and makes treatments like compression, massage, and movement feel worthwhile.
You don’t have to carry the shame, isolation, and exhaustion alone anymore. Our experts at Lymphatic Therapy Services will guide you throughout your recovery journey. Join a lipedema or fat-disorder support group, or find our therapists, who actually understand your condition. You can also connect with our online community. Book your appointment today to start treatment, lighten the load you’ve carried for years, and help you start living again.
FAQs
Why Do Fat Disorders Like Lipedema Affect Mental Health?
The combination of constant pain, easy bruising, heavy limbs, and a body that changes no matter what you do triggers deep shame, grief, anger, and isolation. Years of being dismissed or blamed for a medical condition you didn’t cause leave many with fat disorders feeling worthless, broken, and utterly alone in their struggle.
Can Emotional Support Reduce Physical Symptoms?
Yes, dramatically. Lower stress levels result in lower cortisol and inflammation, which directly reduce pain, burning, and swelling flare-ups. Many women with fat disorders, lipedema, report noticeably lighter, less painful legs within days of finally feeling believed and supported. This is proof that emotional care is real medicine for the body, too.
Are Support Groups Helpful for Fat Disorders, Such as Lipedema?
Yes, they’re often life-changing. Finally talking to women with the same legs, same bruises, and same doctor battles ends years of loneliness in one meeting. Members swap real tips, trusted doctors, emotional coping tools, and genuine hope. Most people say joining a support group was the best decision they ever made for their fat disorder lipedema.
How Can Family Members Support Someone With A Fat Disorder?
Listen without judgment or diet advice, learn the real facts about the condition, believe the pain is genuine, and offer practical help when asked. Simple acceptance, love, and showing up exactly as they are mean everything to someone exhausted from fighting both the condition and the world’s misunderstanding of fat disorders.