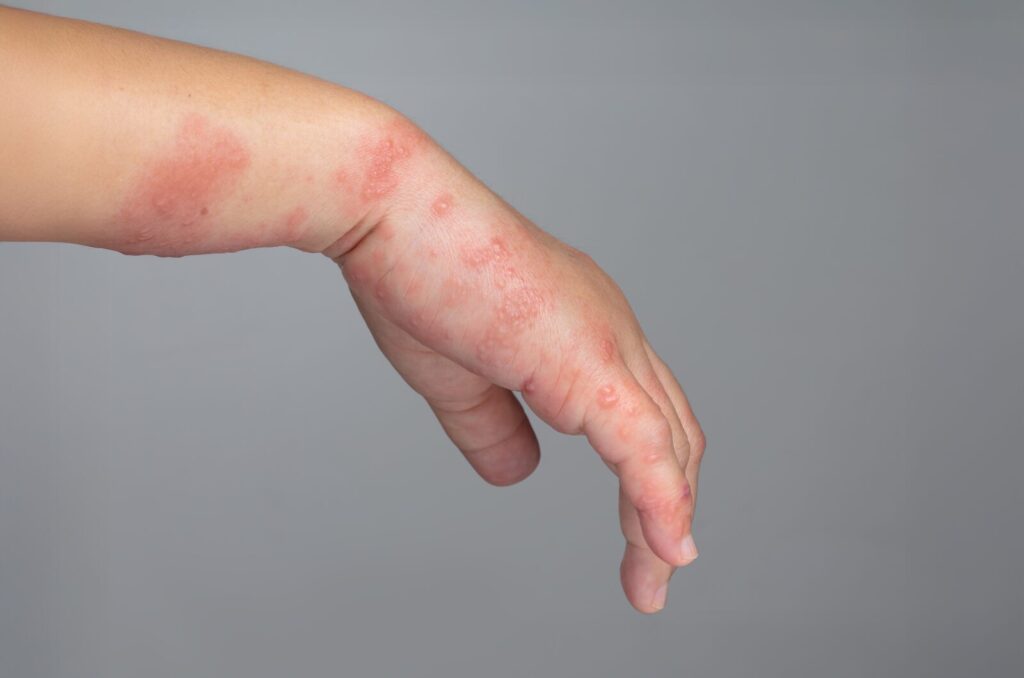
Lyme disease is contracted and spread through the bite of an infected tick. Tiny black-legged ticks bite and pass on bacteria, causing the infection. Lyme disease affects your skin, joints, heart, and sometimes your brain. It starts with mild symptoms and gets worse if not treated early.
Knowing about the different Lyme disease stages helps you understand how the illness grows and changes in your body over time. This article discusses the signs to watch for, Lyme disease progression, and why early diagnosis is important, especially for people living in San Diego, where ticks are common.
What are the Stages of Lyme Disease and How Do They Progress?
The stages of Lyme disease are the early localized, early disseminated, and late disseminated stages. Lyme disease progression happens as the infection spreads through the body if left untreated, moving from the initial site of the bite to other organs and systems. Each stage has different symptoms and risks, making it important to recognize and treat the disease early.
Early Localized Lyme Disease: Initial Infection and Symptoms
Early localized Lyme disease is the first stage that occurs days to weeks after a tick bite. At this point, bacteria multiply near the bite site, causing a distinctive red rash shaped like a bull’s-eye called erythema migrans. This rash is a key sign, but it may not appear in everyone.
People can also experience flu-like symptoms such as fever, chills, headache, and muscle aches. The infection is still confined mainly to the skin during this stage, making it easier to treat. Prompt antibiotic therapy is effective and can prevent the disease from progressing further. Recognizing these early signs is critical since early localized Lyme disease begins the progression of Lyme disease.
Early Disseminated Lyme Disease: Spread of Infection in the Body
If early localized Lyme disease is untreated, the infection can spread throughout the body, entering the early disseminated stage. This occurs weeks to months after the initial tick bite. During this phase, the bacteria reach the heart, nervous system, and other organs, causing new symptoms.
Patients may develop multiple rashes, facial palsy (weakness or drooping on one side of the face), severe headaches, or heart irregularities such as Lyme carditis. Other common signs include fatigue, joint pain, and swelling.
Because the bacteria are spreading, symptoms may seem unpredictable or come and go. Early disseminated Lyme disease requires timely medical attention to prevent serious long-term issues and helps illustrate why understanding Lyme disease progression is so important.
Late Disseminated Lyme Disease: Chronic Symptoms and Complications
Late disseminated Lyme disease represents the final stage and appears months to years after the initial infection if it remains untreated. At this point, the bacteria have caused widespread damage, particularly to joints and the nervous system.
Chronic symptoms may include persistent joint pain or swelling in the knees, neurological problems such as memory issues, numbness, difficulty concentrating, and heart problems. Some individuals may experience fatigue and muscle weakness long after treatment begins.
This stage severely affects a person’s quality of life if not addressed promptly. Understanding the severity of late disseminated Lyme disease highlights the need for early recognition of Lyme disease stages to stop progression before serious harm occurs.
How to Recognize Symptoms at Each Stage of Lyme Disease
The symptoms of Lyme disease vary across its stages. In early localized Lyme disease, symptoms mainly include a rash and flu-like signs. As the disease progresses to the early disseminated stage, symptoms become more diverse and can affect the nervous system and heart.
Late disseminated Lyme disease brings chronic symptoms such as joint pain and cognitive issues. Recognizing these symptoms early in each stage is vital to managing the disease and avoiding complications.
Identifying the Early Erythema Migrans Rash and Flu-like Symptoms
The earliest and most common symptom in the first stage of Lyme disease is the erythema migrans rash. This rash is round and expands over days, sometimes resembling a bull’s-eye, although it can vary in appearance. It appears at the tick bite site within 3 to 30 days.
Alongside the rash, many people experience flu-like symptoms such as fever, chills, headache, fatigue, muscle aches, and swollen lymph nodes. These symptoms indicate the body’s immune response to the bacteria. Early recognition of these signs is crucial, as antibiotics started during this stage can stop further Lyme disease progression and prevent long-term effects.
Neurological and Cardiac Symptoms in the Disseminated Stage
In the early disseminated stage, symptoms become more serious as the infection spreads through the bloodstream to different body parts. Neurological signs may include facial palsy—weakness or drooping on one side of the face—severe headaches, neck stiffness, and sometimes numbness or tingling in the limbs.
Struggling with swelling, fatigue, or post-surgery recovery?
Book your personalized lymphatic drainage session today and experience natural, therapeutic healing that restores balance and promotes long-term wellness.
Book an AppointmentCardiac symptoms like irregular heartbeat or palpitations, known as Lyme carditis, may also occur. Fatigue and muscle or joint pain become common. These symptoms reflect lymph disease progression beyond the initial site and need prompt evaluation and treatment to avoid permanent damage to the nervous system or heart.
Joint Pain, Cognitive Issues, and Long-term Effects in the Late Stage
Late disseminated Lyme disease stage presents with ongoing joint pain, especially in the knees. This arthritis becomes chronic and severely limits mobility. Neurological symptoms such as memory problems, numbness, difficulty concentrating, or tingling may also appear or worsen.
Some individuals suffer from persistent fatigue, sleep difficulties, or mood changes. These long-term effects are the result of Lyme disease progression that was not treated or controlled earlier. Timely treatment in earlier stages prevents these chronic complications, emphasizing the importance of recognizing symptoms at every stage.
Why Early Diagnosis and Treatment are Crucial in Lyme Disease

Early diagnosis and treatment are crucial in Lyme disease because they stop the infection before it spreads and causes serious damage. Treating Lyme disease promptly helps prevent symptoms from worsening or becoming chronic.
It also reduces long-term complications affecting the joints, heart, and nervous system. Early care lowers the chances of expensive, lengthy treatments later on.
How Timely Antibiotic Treatment Prevents Disease Progression
Early antibiotic treatment during the initial Lyme disease stages is key to preventing the infection from advancing to more severe phases. Antibiotics promptly kill the Borrelia bacteria before they spread beyond the skin to the heart, nervous system, or joints.
This stops Lyme disease progression and reduces symptoms quickly. Delayed treatment may mean more intense symptoms and longer recovery times.
The Role of a Lyme Disease Treatment Center in San Diego
A specialized Lyme disease treatment center in San Diego is important in managing all Lyme disease stages and progression. These centers have expertise in recognizing symptoms early and providing accurate testing, which can sometimes be challenging. They offer personalized treatment plans depending on the stage of infection and the individual’s needs.
Such clinics also provide follow-up care to monitor recovery and address any ongoing symptoms. For San Diego residents, access to a local treatment center helps ensure prompt diagnosis and effective management to prevent Lyme disease progression and improve overall outcomes.
Conclusion
Lyme disease stages show how the infection changes and worsens if not treated quickly. Understanding Lyme disease progression helps you recognize symptoms early, seek proper care, and avoid serious complications.
Early diagnosis and treatment are the best ways to protect your health and stop the disease from advancing. If you live in San Diego and think you might have Lyme disease symptoms, do not hesitate. Reach out to a healthcare provider or Lyme disease treatment center right away. Taking action early can make all the difference in your recovery and long-term well-being.
FAQ’s About Lyme Disease
Can Lyme disease skip stages or show overlapping symptoms?
Lyme disease progression usually follows distinct Lyme disease stages, but it can sometimes show overlapping symptoms, making it hard to identify a clear stage. Some people may experience symptoms from multiple stages simultaneously, especially if treatment is delayed.
While the disease rarely skips stages entirely, the symptoms’ timing and severity can vary, so understanding Lyme disease progression helps recognize and manage such cases effectively.
What are the most common neurological symptoms of Lyme disease?
Common neurological signs include facial palsy (muscle weakness on one side of the face), severe headaches, neck stiffness, numbness, tingling sensations, and sometimes memory or concentration difficulties.
Neurological symptoms appear during the early disseminated and late Lyme disease stages as part of Lyme disease progression. These symptoms indicate the bacteria have affected the nervous system and highlight the importance of early diagnosis in preventing serious complications.
Can untreated Lyme disease cause permanent health problems?
Yes, untreated Lyme disease can lead to permanent health problems due to continued Lyme disease progression through its stages. Without timely treatment, the infection can cause chronic joint pain, neurological issues like memory loss or numbness, and heart complications. Early recognition and treatment of Lyme disease stages are crucial to improving recovery chances and preventing long-term damage.
How is Lyme disease diagnosed if symptoms vary widely?
Diagnosing Lyme disease requires careful evaluation because symptoms often overlap or vary across Lyme disease stages. A Lyme disease specialist San Diego relies on patient history, possible tick exposure, symptom patterns, and blood tests to detect the bacteria.
Understanding Lyme disease progression helps providers interpret test results and symptoms together, ensuring accurate diagnosis despite varied clinical presentations. Early diagnosis is key to effective treatment.